To know more about our Office Hysteroscopy program, please write to us at reachus@corionfertilityclinic.com
 What is Office Hysteroscopy?
What is Office Hysteroscopy?
Office hysteroscopy is performing a hysteroscopy on an out-patient basis. That is, a patient can walk in the clinic, the doctor performs a hysteroscopy without anaesthesia and the patient can walk out of the clinic almost immediately and can resume normal activities immediately.
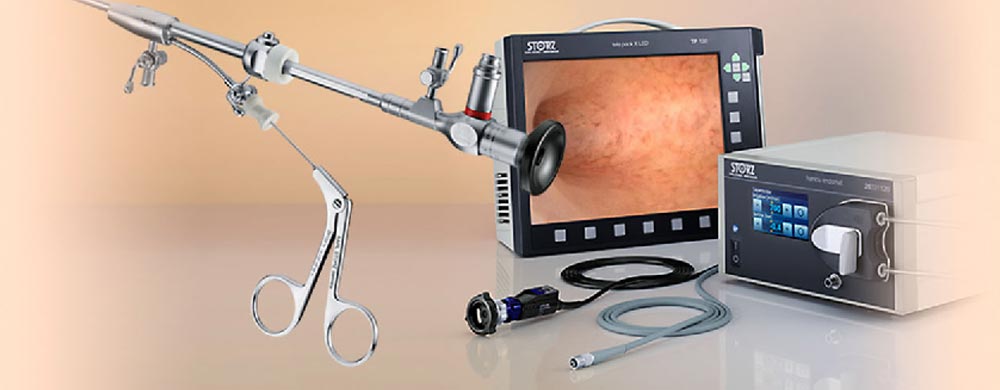
An office hysteroscope is a thin, lighted telescope-like device. It is inserted through the vagina and the cervix into the uterus. The hysteroscope transmits the image of your uterus onto a screen. It is used to visualise the lining of the walls of the uterine cavity. Other thin instruments are used along with the hysteroscope for treatment.
A regular hysteroscope is of 4mm diameter. The office hysteroscope is of a smaller diameter of 2.9 mm. Since it is of a smaller diameter, the procedure can be performed without anaesthesia as there is no need to dilate the cervix. It might however, require local anaesthesia in the cervix.
It is similar to undergoing an internal pelvic examination.
One of the most common uses for hysteroscopy is to find the cause of abnormal uterine bleeding. Abnormal bleeding can mean that a woman’s menstrual periods are heavier or longer than usual or occur less often or more often than normal. Bleeding between menstrual periods also is abnormal.
Most of the procedures can be done without general anaesthesia. However, a local anaesthetic may be given and then a tiny telescope with a camera is placed through your cervix into the uterine cavity. A sterile saline solution is instilled into the uterus so that you can see the walls. We have the latest in office hysteroscopy equipment, including a 2.9 mm hysteroscope which results in significantly less patient discomfort compared to the conventional 5 mm hysteroscope. Since the patient is awake, she can watch the procedure on the monitor.
To know more about our Office Hysteroscopy program, please write to us at reachus@corionfertilityclinic.com
Many women feel some cramping, especially when the sterile saline solution is instilled. Women with blocked fallopian tubes may feel more uncomfortable. Even though we are using the smallest hysteroscope available. We do recommend that one hour before the procedure you take pain killer pills as advised by the doctor.
Many women have no pain after the hysteroscopy, but you may feel a little cramping. You should be able to return to work after the procedure. It is normal to have some mild cramping or a little bloody discharge for a few days after the procedure. You may be given medication to help ease the pain. If you have a fever, chills, or heavy bleeding, call your health care provider right away.
You should call the office with the first day of menses so that we can schedule the test. The hysteroscopy is usually scheduled after your period ends, but before you expect to ovulate, usually between days 6-12 of your menstrual cycle. You need to use protection during intercourse prior to the test. You may resume intercourse without protection 24 hours after the procedure.
Copyright © 2024, Corion. All Rights Reserved.
Website is designed & developed by Phi Brands