Blastocyst Transfer
At Corion, IVF laboratory is proficient at blastocyst culture
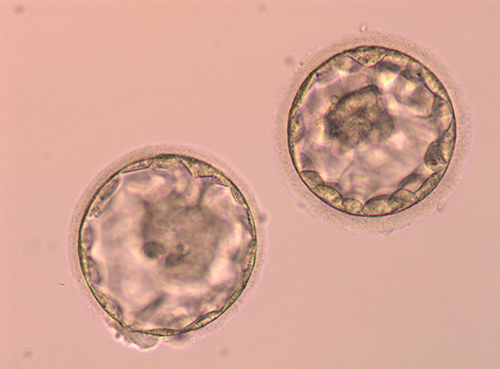
- Our IVF laboratory has excellent quality controls and is therefore able to do a day 5 blastocyst transfer
- A blastocyst is an embryo that has been allowed to develop in the laboratory for five or six days after egg collection. This is in contrast to standard IVF where embryos are only allowed to develop up to day two or three in the laboratory, before being transferred to the uterus
- The outer sphere of the blastocyst is called the Trophoblast
- The inner portion of the blastocyst is filled with fluid
- Inside the trophoblast, there is a clump of cells called the Inner Cell Mass (ICM). The inner cell mass is the portion of the blastocyst that actually becomes the baby
- Only a small percentage of embryos will reach the blastocyst stage. This self-selection of the embryos allows the embryologist to pick the embryos that are most likely to produce a pregnancy
- While transferring blastocysts, fewer embryos are transferred as compared to day2 embryos. This reduces the risk of multiple pregnancy
- Major potential benefit of transferring blastocyst following IVF is reduction of the possibility of multiple pregnancies
- This is true for all age groups
- The rationale behind a blastocyst transfer is that an embryo that has failed to reach the blastocyst stage would be unlikely to have resulted in a pregnancy. However, if it reaches the blastocyst stage it has about 50% chance of implanting. So the improved implantation rates following blastocyst transfer is due to selection of the best embryos
- Two main reasons why 50% blastocysts fail to implant: A defective blastocyst (e.g. chromosomal abnormalities) or non-receptive endometrium
- However, if the culture environment is suboptimal, delayed embryo development and even embryonic arrest will occur
Blastocyst transfer is recommended for:
- Couples who have repeatedly failed to achieve a pregnancy following the transfer of good quality cleaved embryos (If the embryos arrest and do not develop to a blastocyst, this may indicate a potential egg problem)
- Couples who wish to achieve a pregnancy without the risk of multiple pregnancies
- Couples who do not wish to have their spare embryos frozen
Frozen Blastocyst Cycles
- Blastocysts have a very good survival rate after cryopreservation (freezing). The recovery after thawing is equivalent to that of thawing at earlier embryonic stages
- Blastocysts are superior to earlier stage embryos in terms of development. They are also easier to freeze, store, and thaw
OUR SERVICES:
Sperm DNA Fragmentation Ovarian rejuvination Thin Endometrial Lining PGS (PGT-A) & PGD (PGT-M) Cryopreservation / Fertility Preservation / Vitrification Egg Freezing / Oocyte Cryopreservation Sperm Cryopreservation Vitrification & Frozen Embryo Transfer Recurrent Pregnancy Loss IUI-Intrauterine Insemination Blastocyst Transfer Laser Assisted Hatching Follicular Monitoring TESA-Testicular Sperm Extraction PESA – Per Epididymal Sperm AspirationCopyright © 2024, Corion. All Rights Reserved.
Website is designed & developed by Phi Brands


